The Wisdom Found in the Oncology Center
You don’t have to go very far to find someone who would trade places with you. The children’s oncology ward is just one floor down.
May 2022
Howdy everyone. It’s been almost 8 weeks since I had emergency spinal fusion surgery, avoided paralysis, and was diagnosed with stage 1 multiple myeloma- a bone cancer. I have started month 2 of an 8 month oncology treatment which includes chemotherapy, radiation, and later, a stem cell (bone marrow) transplant. Overall, it goes well.
In the second half of May, I have 25 medical appointments scheduled over 2 weeks. This is a lot of time in oncology waiting rooms, talking with doctors and nurses, and getting treatments. It’s a lot of time thinking and talking about cancer. There is certainly a technical part that I’m focused on: understanding lab results, managing side effects, physical therapy, how radiation works, and the sheer logistics involved in getting places and taking lots of pills. In between these conversations, I sit back and take it all in. I’m in the MGH oncology center waiting room with dozens of other people at various points in their journey. I hear advice from expert caregivers. I’m hearing my infusion neighbor speak to the nutritionist, and I learn and admire her spirit in the process. There is a lot of wisdom to be found in an oncology clinic.
I’m writing this to help myself make sense of it all. There are lessons I’m learning that I want to remember clearly going forward. I hope some of them may be useful to you, though, god willing, not as an oncology patient yourself.
A Framework for Making Sense of a Cancer Diagnosis
My approach to ambiguous and open-ended situations like this is to zoom out, map the entire system, and place myself in it as objectively as possible. By seeing where I am and where I could be going, and how to get there, I become grounded. It is easier to see what I need to do, and with what mindset. While it is easy to fixate on the nuisance chemo side effect of the day, zooming out reminds me of three things:
There are many options which lead to a good outcome.
Keep expectations closely matched with reality.
Things could always be much worse. Be grateful. Other people would love to have your problems.
In every case for me, having more knowledge of objective reality, broader and longer perspective, and understanding the full spectrum of human experience beyond my own makes my own problems smaller and easier to deal with. I’m not suggesting I’ve reached any sort of enlightenment or mastered stoicism. I’ve had moments of frustration in the past few weeks, and that is normal. Mapping out reality and figuring out the likely path I’m on is simply what works for me. Every person is wired differently, and each person’s cancer and response to treatment is difficult to predict.
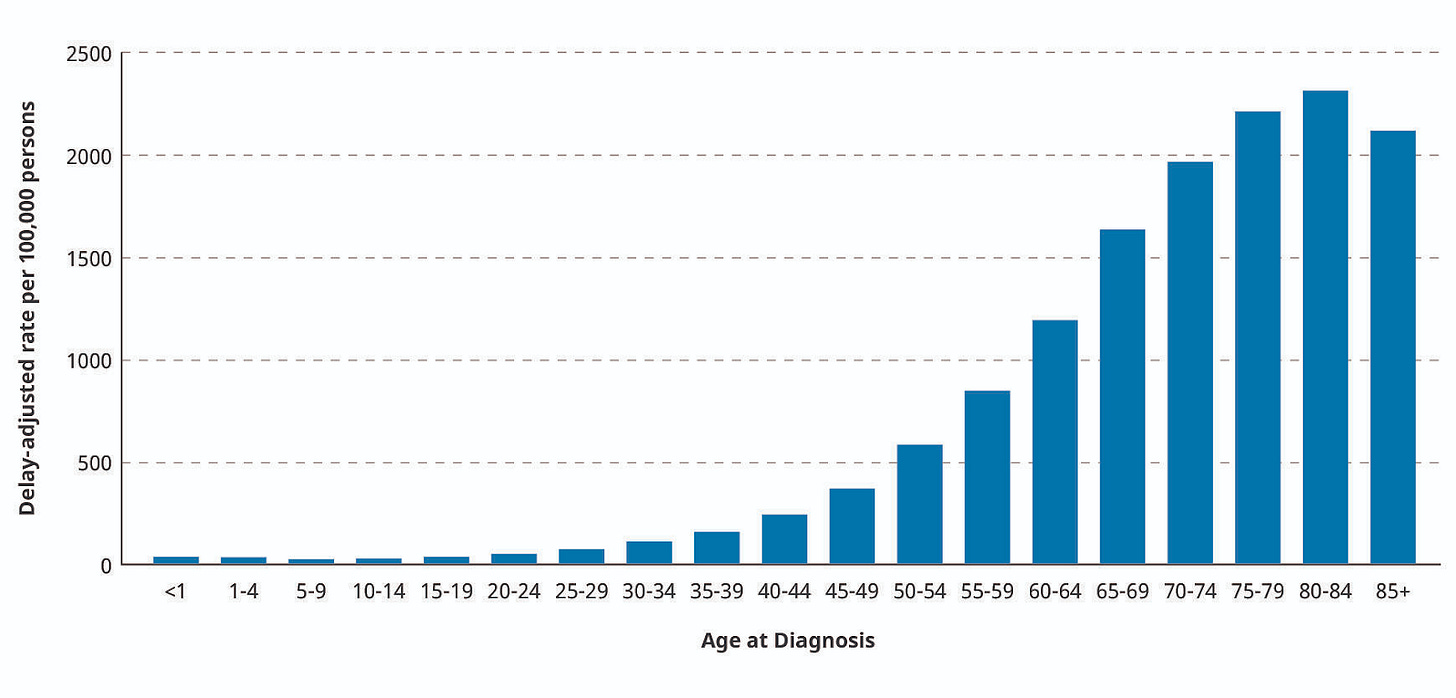
The latest statistics show that 1 out of every 2 women and 1 out of every 3 men will get cancer sometime in their lifetime. The chart below is instructive. When, god forbid, you or someone you care about gets diagnosed with cancer, it is usually later in life (>60). Steady improvements over the past 50 years in healthcare and science means that our healthcare systems are able to deal with many ailments that would have struck you down earlier, should you be so fortunate to live in such a system. As a result, we have been steadily uncovering the conditions that are hard to deal with: Alzheimer's, cardiac failure, cancer etc. Even some of these hard-to-deal-with ailments are becoming manageable chronic conditions. It is not easy, but it is not a death sentence.
The Patient Perspective
If you are like me, you’ve fortunately not had to deal with cancer up close for most of your life. Maybe a relative was diagnosed and recovered. Maybe a friend’s aunt lost her ongoing battle. Soon after you get diagnosed, you might see the world in a few paths:
In summary:
Path A: Science is great. People are smart. I’m going to be fine. I better be fine.
Path C: Fuck. This could be really bad. I hope they tell me point blank if it’s that bad.
Path B: Somewhere in the middle between A and C. Start googling.
While you want to ask, “how much longer do I have?”, you also know that you generally don’t want to know the answer, so you don’t ask. If the answer is a long long time, the oncologist doesn’t know this yet and can never say for certain. If the answer is very short because you have stage-4 metastasized cancer for which there are not great therapies, this is not what you want to hear. More data will come in the next 1-2 weeks which can tell you if you are on path A or C, or at least rule out path C if you should be so lucky. As the biopsies, CTs, pathology results and lab work starts to come back, the oncology care team can start to give you some direction information. It’s either A/B, or B/C.
Until then, some human on the oncology team needs to tell the patient something. Enter Dr. Jeffrey Clark, a senior attending oncologist in hematology (blood cancers) at Mass General Hospital. While I was in the emergency room hallway waiting for surgery, Dr. Clark and his resident came by several times that morning to introduce themselves to me, and take my story. What I did not realize at the time was that as much as they were trying to corroborate their hypothesis that I had multiple myeloma, they were also building a psychological portrait to figure out how to best to tell me what I needed to hear. They had an MRI, blood lab results, and my story. I don’t remember exactly what words Dr. Clark used, but it made sense, and it was a pill I could swallow. In retrospect, this conversation required a lot of wisdom on his part. I do not think this wisdom is taught and learned in any medical school course or textbook, but rather accumulated through a lifetime of conversations and understanding the broad spectrum of how humans deal with having their world turned upside down. I appreciate that every doctor needs to give bad news to patients. In oncology, there’s often not a lot of great news to go around.
There is a certain amount of hope and optimism that is healthy, and then there are just false hopes that set the patient up for a greater spiritual fall.
Happiness = Reality - Expectation
Every person has a range of reality-minus-expectation gap that they can deal with. Dr. Clark has seen it all and had this conversation hundreds of times. My take-away was that there is a lot that is unknown right now, but once things start falling into place, there is a lot that can be done by an expert team. He said to focus on getting through the spine surgery, and they’ll know a lot more soon about what they suspect is myeloma. Fair. Even though they had no solid answers, I was glad to meet the kind of thoughtful humans who would be figuring this out for me.
The Oncology Care Team Perspective
A team of oncologists specializing in spine and multiple myeloma cancer knows the lay of the land well. Multiple myeloma is a complex cancer often involving every bone in the body, and blood which circulates to every system. Certain organs and systems may already be stressed due to being overloaded with byproducts made by myeloma cells. Instead of my low resolution map of A/B/C, their map is far more nuanced, with onramps and off-ramps between paths. They’ve seen miracles where long odds were beat, and tragedies where normal cases deteriorated. Nothing is a slam dunk, but it is okay to be optimistic and upfront around a reasonable set of outcomes.
This map bears some explanation:
A better life outcome is one where your post-cancer lifespan is close to your pre-cancer life expectancy for yourself, and most of those decades or years are cancer-free. The treatment is but a bump in the road.
If you have a cancer recurrence after you thought you were in remission, the next round of treatments tend to be more difficult to endure. Hence the lower quality of life with sequential treatments.
For the A1, A2, A3 paths, you may not need to make too many adjustments to your outlook and lifestyle. You will regain most of it, and have plenty of time to enjoy it.
For the A4, B1 paths, you still have plenty of time, but may need to make some lifestyle modifications. It is not as care-free.
For B2, B3, your life will be shorter than you planned, but you still have time. Walter White was on these paths.
For the C paths, your options are limited. Balancing quality of life and total time left is a difficult equation. Let the patient be in as much control for as much time as possible.
As most cases are not solved by slam dunks, the oncology care team needs to prepare the patient for a long fight. I define a long fight as one that lasts many months or years, draining you of energy along the way, and success is not guaranteed. Apart from labs and baseline health data, the oncology team knows that cancer is not easily fought alone. It requires the patient to be grounded in reality and deal with what is at hand, and this may change every week. For the long fight, patients need to manage energy reserves and their own frustration level. Stubbornness and grit are helpful, to a point. Beyond that point, these qualities are counterproductive and even risky. For me, this comes down to having an accurate mental model of how things will play out, and manage what is within my control. Minimize the gap between expectation and reality, and make the most of the current reality. I think that is the healthiest way to adapt over a long fight, but am open to other approaches. The long fight isn’t just getting through treatments. It’s recognizing that it’s worth sacrificing short term quality of life to achieve remission as quickly as possible, and live as much time cancer-free and care-free as possible. I have made clear to my care team that I am on board with this approach, and will hold up my end.
The oncology team by now has pieced together a decent whole person profile of me, and knows I have lots of support from family and friends, and my workplace. We’re not under financial hardship. I’m decently well-educated in science and have a lot of curiosity, do research, and take notes. What they did not know at this point was:
How quickly is my cancer growing? Is it an aggressive form?
Are other organs and systems at risk, which might delay full chemotherapy?
Is my cancer normal? What will the biopsy and bone marrow draw show?
How will I respond to chemotherapy? Will I have an allergic reaction?
Will the labs show the normal myeloma response to chemotherapy?
Despite my outwardly good attitude and energy, do I have the deep resilience for the long fight?
Only time and treatments will tell. There is no crystal ball for this. Fortunately, most of these data points have come back positive, and A2 or A3 are viable paths.
As I recovered from surgery in the oncology ward, the medical director of the MGH Hematology Cancer Center, Dr. Robb Friedman, came in for a long chat. I didn’t have enough context to put together the chart above, but this conversation and the ones that followed certainly helped fill out the map. In both a humble and expert way, he explained different therapy options, how quickly the therapies are improving, and how such options are causing hematology teams to rethink their approach to give patients the best outcomes. By this point, I’d started to learn more about multiple myeloma, chemotherapy, and what the next 6 months might be like. I gathered that I was on the A/B path, and not the C path. Recent lab results and further scans confirmed this. As of this writing, I’m somewhere on the path between A2 and B1. I’ll take it. I give Dr. Friedman a lot of respect for being able to have these conversations with patients he’s just only met, regardless of what likely paths he sees them on. Oncology care teams are a special type of medical professional.
The Oncology Waiting Room
I’ve become aware that in every oncology waiting room I go to, I’m the youngest patient by 1-3 decades. (One floor down there is the pediatric oncology ward and clinic.) This is hard to write. Everyone in the room is wondering how much longer or shorter their life will be, which path they are on. Some do not have much time left at all. Half the waiting room is probably not going to get good news today. They are not going from C1 to A4. Most people don’t look like oncology n00bs like me, and have been coming for a while. This tells me they are probably in the B range. I think 80% of them would want to trade health and cancer diagnosis with me. Stage 1 multiple myeloma in a young otherwise healthy person with lots of promising therapies gives a lot a hope to hang on to. This means the oncology staff are generally dealing with people facing really long odds, which makes their humanity and unending empathy even more impressive.
Last week I finally saw a young man about my age in the waiting room. He brought multiple generations of family with him, likely to meet the oncologist for the first time. Our exam rooms were across the hall from each other, and both doors open; his door because family spilled out into the hallway, mine because I’m nosy and every room is always more interesting with an open door. I heard a few familiar words: “myeloma,” “chemo has come a long way,” “we’ll start right away.” I so hope that they caught his cancer early and was happy to see he was surrounded by a loving family. I hope his spirit burns bright when no one else is around. He and I both get to be treated at MGH (Man’s Greatest Hospital).
Oncology Treatment
Every oncology doctor, physical therapist, nurse, tech, and staff member I’ve met at MGH has been excellent. They are expert, kind, good humans. It makes these appointments a pleasure. Joe, who takes my blood pressure, does so with enviable energy and a warm smile. I enjoy learning from deep experts and people with lots of skills in their hands. Most of all, they care about me as a whole person. They always ask how Julia and the boys are doing, and how I am staying sane. They mean it when they ask, and their post visit notes reflect it. They know that cancer recovery is a mental game, and one that requires a community to keep the patient’s identity on solid ground. I am so grateful for this highly evolved part of our medical system. I take pride in bringing my best self to meet with these teams. My physical therapist who specializes in oncology patients says that they are by far the best, nicest, most grateful patients: they see every day as a gift.
Final Thoughts
Most of this can apply to any chronic condition: mental illness, chronic pain, or incurable ailments. If there’s any tangible advice that I’ve gleaned from the past couple months, it is this (in no order).
Don’t sweat the small stuff. Most of it does not matter. Ask yourself at what age you will have forgotten about this thing that bothered you today, and why that can’t be tomorrow.
Have grace. Someone might have just found out they went from B2 to B3, or are 2 years into caring for a loved one on path C2. They might never let you know. Carry yourself in a way that they can talk to you about it if they need to.
If you are fortunate enough to be on an A or B path where you have plenty of time left at some quality, treat it as a gift. Maybe give a gift to someone you care about. A gift may be letting go of that which has been dragging you down for too long. Unburden your life so you can focus on the people and pursuits that matter.
You don’t have to go very far to find someone who would trade places with you. The children’s oncology ward is just one floor down.
Even on a day when you are feeling like a bag of broken dicks, you can still stand tall with your indomitable spirit.



This is my very first Substack comment posting. Not sure why that was relevant to share? Perhaps it”s relevant because posting comments is not something I ever do. Why? I just can’t put my thoughts down on paper in a witty and interesting way that would motivate one to stay up late in bed and read them like I just did with your post. (Insert some witty and funny analogy that Jason would use here to illustrate how much I enjoy reading what he shares. But since I am not him, I’ll just write… ). I love reading what you share! And I hope you continue to write and share what is in that mind of yours.
Btw, I loved The Good Place reference and I am curious if you have actually watched it? Maria and I starting binge watching it and eventually I stopped but she didn’t. So if you have seen it, maybe that will be a future topic? :)
Keep writing my friend and I’ll keep praying. I am grateful you are on the A-B side of things.
Look forward to your next post!